

The Vanden Berghe Lab is a multidisciplinary team performing basic as well as applied research on mechanisms, treatment and prevention of cell death-driven diseases, with focus on ferroptosis (kind of biological rust). We follow an integrated approach from knowledge building and discovery to (pre)clinical research, along support and consultancy.
Multiple organ dysfunction syndrome (MODS) accounts for 30% of global intensive care unit (ICU) deaths, with reactive iron playing a key role in driving ferroptosis-induced cell death and organ failure in critical illness. In collaboration with the Augustyns lab, we have developed, characterized, and patented novel ferroptosis inhibitors with superior efficacy, solubility, and stability. Among more than 200 analogues, we identified three lead candidates with significantly improved properties over existing benchmark inhibitors. These candidates demonstrated strong protective effects in multiple ferroptosis-driven disease models, with one exhibiting unprecedented, life-saving efficacy against experimental MODS. To accelerate clinical translation, we are launching IRONIX, a ferroptosis-focused therapeutic spin-off, in Q1 2025. Alongside drug development, we are designing a companion diagnostic test to enable patient stratification, ensuring targeted and effective treatment for MODS patients.
The success of organ transplantation is limited by a shortage of viable grafts and the damaging effects of ischemia-reperfusion injury (IRI). During IRI, activation of the innate immune system triggers inflammation and cell death, contributing to primary graft dysfunction (PGD)—a major risk factor for both early and late transplant-related morbidity and mortality. To expand the pool of usable organs, ex vivo perfusion strategies have been developed, offering a critical window for graft optimization. Machine perfusion, in particular, provides a unique opportunity to counteract ferroptosis-induced damage before transplantation. Our proprietary and patented ferroptosis inhibitor has demonstrated superior efficacy in preclinical models of organ injury, positioning it as a promising therapeutic candidate to enhance graft survival and improve transplant outcomes.

In patients with sepsis or multiple organ dysfunction syndrome (MODS), elevated plasma labile iron levels and excessive inflammasome activation are critical drivers of mortality. Ferroptosis, triggered by iron overload, plays a key role in organ damage, yet the considerable variability in MODS and sepsis—shaped by genetic differences, comorbidities, frailty, and dynamic disease progression—complicates treatment strategies. To enable more precise patient stratification, there is an urgent need for predictive biomarkers that can distinguish clinically similar patients into distinct subtypes. To address this challenge, we combine genetic models of ferroptosis-induced kidney, liver, and brain injury with biofluid analysis from critically ill patients to identify ferroptosis signatures. Our approach includes developing immuno-based bead arrays to detect ferroptosis-related factors released by dying cells and leveraging Nanopore (epi)sequencing of cell-free DNA to uncover signs of tissue injury and ferroptosis. Because cfDNA carries CpG methylation patterns that reflect both the tissue of origin and the epigenetic state of dying cells, it offers a promising avenue for integrative, minimally invasive diagnostics. By integrating precision medicine with cutting-edge molecular diagnostics, we aim to revolutionize intensive care practices, paving the way for targeted and personalized therapeutic interventions.

Multiple sclerosis (MS) is a chronic autoimmune disorder driven by central nervous system inflammation and demyelination, fueled by a self-perpetuating cycle of inflammation and cell death. Analysis of MS lesions and cerebrospinal fluid has revealed key ferroptosis markers, including elevated labile iron levels, peroxidized phospholipids, and lipid degradation products. In a preclinical model of relapsing-remitting MS, treatment with our lead ferroptosis inhibitor significantly delayed relapses and slowed disease progression, highlighting its therapeutic potential. Stroke, a leading cause of disability and mortality worldwide, lacks effective acute therapies despite its immense global burden. Emerging evidence suggests that ferroptosis contributes to stroke pathogenesis, making it a promising target for intervention. Our research aims to develop and evaluate novel ferroptosis inhibitors capable of crossing the blood-brain barrier to mitigate stroke-induced brain injury. By targeting this critical pathway, we seek to advance innovative treatment strategies for both MS and stroke, offering new hope for patients with these debilitating neurological conditions.
Neuroblastoma is the most common extracranial solid tumor in infants and young children. The high-risk variant is particularly aggressive, marked by poor prognosis, therapy resistance, and a high likelihood of relapse. To overcome these challenges, novel therapeutic strategies are urgently needed. Our research has identified a promising approach to targeting aggressive, therapy-resistant neuroblastoma in mouse models by inducing ferroptosis—a form of iron-driven cell death akin to biological rusting. By exploiting this vulnerability, we aim to develop innovative pharmacological and nanomedicine-based therapies to enhance ferroptosis efficacy, offering new hope for children battling this devastating disease.
Ferroptosis is emerging as a promising therapeutic strategy for cancer treatment. However, epigenetic modifications have been identified as key drivers of resistance to ferroptosis-inducing therapies, limiting their clinical efficacy. This project seeks to unravel how these epigenetic changes contribute to ferroptosis resistance and explore plant-derived epigenetic compounds as potential tools to reverse these alterations. In addition, the absence of reliable diagnostic tools to predict a tumor’s sensitivity to ferroptosis remains a major hurdle. To address this, we are developing nFERROCATCH, a novel Nanopore sequencing-based assay designed to systematically assess tumor susceptibility to ferroptosis-targeting therapies. By enhancing our understanding of resistance mechanisms and providing a predictive tool for treatment response, this research aims to pave the way for more effective and personalized ferroptosis-based cancer therapies.
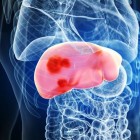
Metabolic syndrome can lead to ectopic fat accumulation in the liver, driving the development of metabolic dysfunction-associated steatotic liver disease (MASLD). With no approved pharmacotherapies currently available, there is a growing need for novel treatment strategies that target cell death-mediated liver injury. Given the association between lipotoxicity, iron dysregulation, and non-alcoholic steatohepatitis (NASH), we investigated the potential role of ferroptosis in MASLD pathogenesis. Our research identified hepatic ferroptosis in a subset of MASLD patients, revealing that ferroptosis defense mechanisms beyond glutathione peroxidase 4 (GPX4) become increasingly prominent in diseased livers. Notably, pharmacological inhibition of ferroptosis effectively slowed MASLD progression in two preclinical models, highlighting ferroptosis as a promising therapeutic target for MASLD.
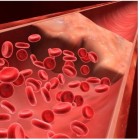
Arterial media calcification (AMC) is a major driver of cardiovascular morbidity and mortality, yet no effective therapies currently exist. This condition not only poses a significant health risk but also imposes substantial economic burdens. Vascular smooth muscle cells (VSMCs) play a central role in AMC pathogenesis, either transdifferentiating into bone-like cells or undergoing cell death in response to oxidative stress. Given the accumulation of iron and lipid peroxidation observed in AMC, we hypothesize that ferroptosis contributes to disease progression. To test this, we will (i) investigate the role of iron in triggering AMC and (ii) genetically induce lipid peroxidation in VSMCs to assess its impact. Finally, we will evaluate the therapeutic potential of our lead ferroptosis inhibitor in preventing AMC development, providing new insights into the role of ferroptosis in vascular calcification and paving the way for novel treatment strategies.

Over the past three decades, chronic kidney disease has risen globally, particularly in agricultural regions, leading to the recognition of Chronic Interstitial Nephritis in Agricultural Communities (CINAC). Despite its growing prevalence, the precise cause and molecular mechanisms driving CINAC remain unclear. However, increasing evidence suggests that exposure to agrochemicals, including pesticides, may play a key role.
In kidney biopsies from CINAC patients, we recently identified lysosomal lesions in proximal tubular cells (PTCs). Notably, similar lesions were observed in transplant recipients treated with nephrotoxic calcineurin inhibitors (CNIs), pointing to a shared toxic mechanism. We hypothesize that ferroptosis contributes to kidney deterioration in these cases, yet the specific toxins and underlying cellular pathways remain unidentified. To address these gaps, we will analyze renal biopsies from both CINAC patients and transplant recipients, aiming to elucidate the role of ferroptosis and uncover the molecular mechanisms driving CINAC pathogenesis. This research may provide critical insights into disease origins and pave the way for targeted therapeutic strategies.
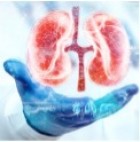
Acute kidney injury (AKI), often triggered by ischemia, toxins, or drug exposure, affects over 13.3 million patients annually, posing a major global health burden. While some cases resolve without lasting consequences, others progress to chronic kidney disease (CKD) due to insufficient repair mechanisms. Despite this, no therapies currently exist to directly promote kidney regeneration. A fascinating phenomenon known as nephrectomy-induced renal recovery offers new insights into kidney repair. This process involves the remarkable regeneration of an acutely injured kidney and the prevention of CKD progression following removal of the healthy contralateral kidney. Emerging evidence suggests that ferroptotic cell death may play a key role in driving efficient kidney regeneration. To unravel the mechanisms behind this process, our research employs single-cell transcriptomics and advanced transgenic mouse models to explore the interplay between cell death and repair pathways. By gaining deeper mechanistic and functional insights, this work aims to pave the way for novel therapeutic strategies to enhance kidney recovery and prevent CKD progression.
A big thank you to…